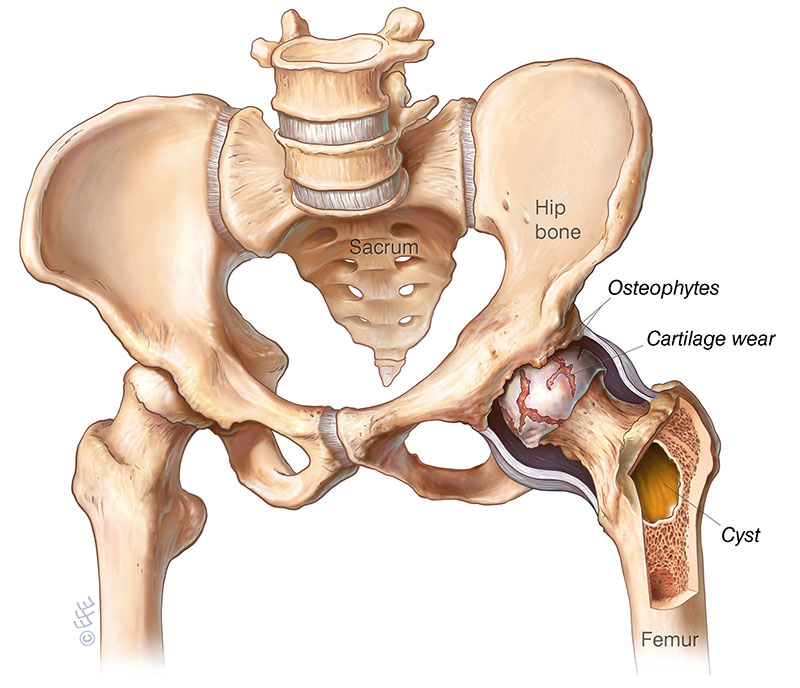
(Figure 1. Cartilage damage seen in Osteoarthritis)
Arthritis of the hip joint is a common condition. It usually affects middle-age and older people resulting in over 40,000 hip replacements being performed in Australia per year to relieve sufferers of their pain. It comes about when the cartilage which overlies the femur (leg) bone or lines the acetabulum (pelvic) bone wears out and exposes “bone on bone” articulation resulting in pain, stiffness and disability.
Many forms of arthritis have been described. Osteoarthritis is the most common form characterized by the break-down of the joint’s cartilage. The exact cause of osteoarthritis is unknown but it may occur in families (genetic predisposition), post-injury or as a result of an infection in the joint.
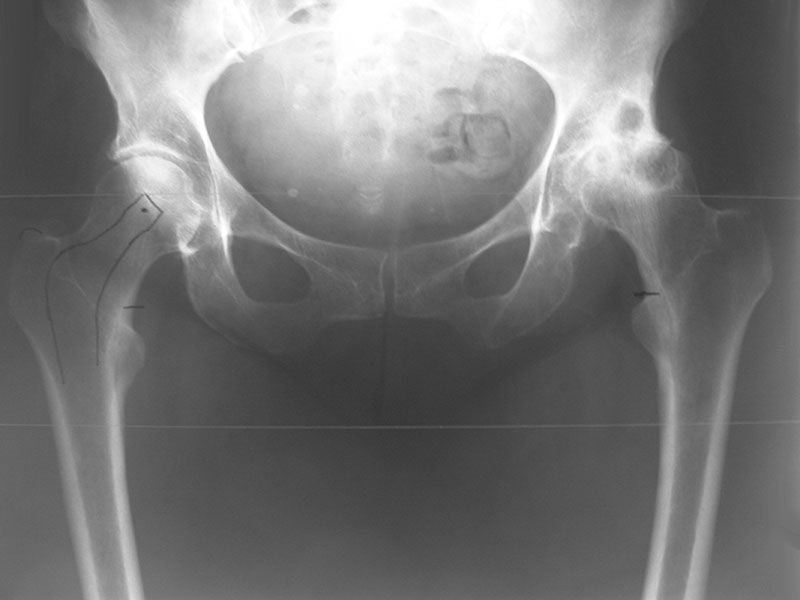
(Figure 2. Severe Osteoarthritis of the left hip)
The next most common form of arthritis is known as rheumatoid arthritis. This is a chronic inflammatory disease of the joint and soft tissues often resulting in the rapid onset of pain, swelling and stiffness with marked joint destruction. Rheumatoid arthritis is more common in women and is caused by the body’s own immune system attacking the joints, often affecting the small joints of the body first i.e. those of the hands and fingers before involving the larger lower limb joints.
Other forms of arthritis are less common and broadly categorized into the term “inflammatory arthritis” including such conditions as ankylosing spondylitis, systemic lupus erythematosus (SLE), gout and juvenile arthritis.
Arthritis of the hip joint often has an insidious onset characterized by the groin, lateral thigh or less commonly buttock pain which may radiate down the leg to the knee and beyond. The pain is worse with activity, limits walking distance and often will cause disturbance of sleep. Early morning stiffness is a common symptom and increases as the disease progresses, often resulting in the inability to reach down to put on one's socks and shoes.
The diagnosis of arthritis is usually made on the basis of the symptom pattern, stiffness and irritability of the joint along with X-ray changes.
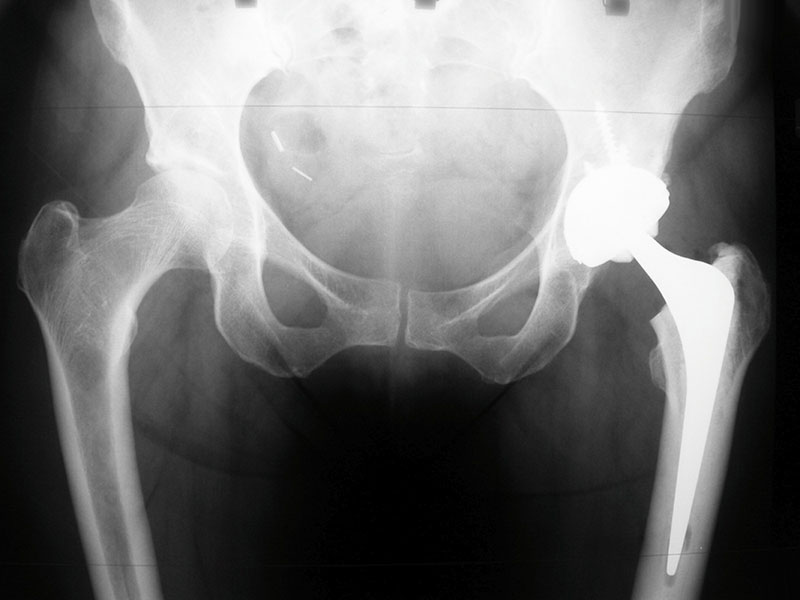
(Figure 3. Left total Hip replacement)
The early management of arthritis involves non-surgical modalities. These include a modification of activities to avoid the aggravating factors e.g. cessation of running / jumping pursuits and substituting those with more suitable activities e.g. walking, cycling or swimming. Weight optimization and the cessation of smoking will increase the lifespan of the remaining cartilage as can dietary supplementation with glucosamines and fish oils. Simple analgesia in the form of paracetamol combined with anti-inflammatory medication is first-line pain control. Physiotherapy and hydrotherapy are used to strengthen the muscles surrounding the joint and walking aids in the form of a stick or frame can make ambulation safer and less painful. A walking stick should be held in the opposite hand to the hip that is affected.
When these first-line measures for managing the pain from your arthritic hip fail to provide effective relief then it may be time to consider hip replacement surgery.
Arthroscopy of the hip joint is a “keyhole” procedure for the treatment of multiple pathologies of the hip joint without large incisions. It allows a faster return to sporting and recreational activities than open procedures, and normally only requires an overnight stay in hospital.
INDICATIONS
Pain in the hip and groin region may be due to many pathologies both inside and outside the hip joint itself. Common pathologies seen inside the joint are cartilage tears, loose bodies, bony bumps that cause impingement-cam or pincer (Figures 1 and 2), inflammation of the joint lining and tears of the ligaments that provide the joint with stability.
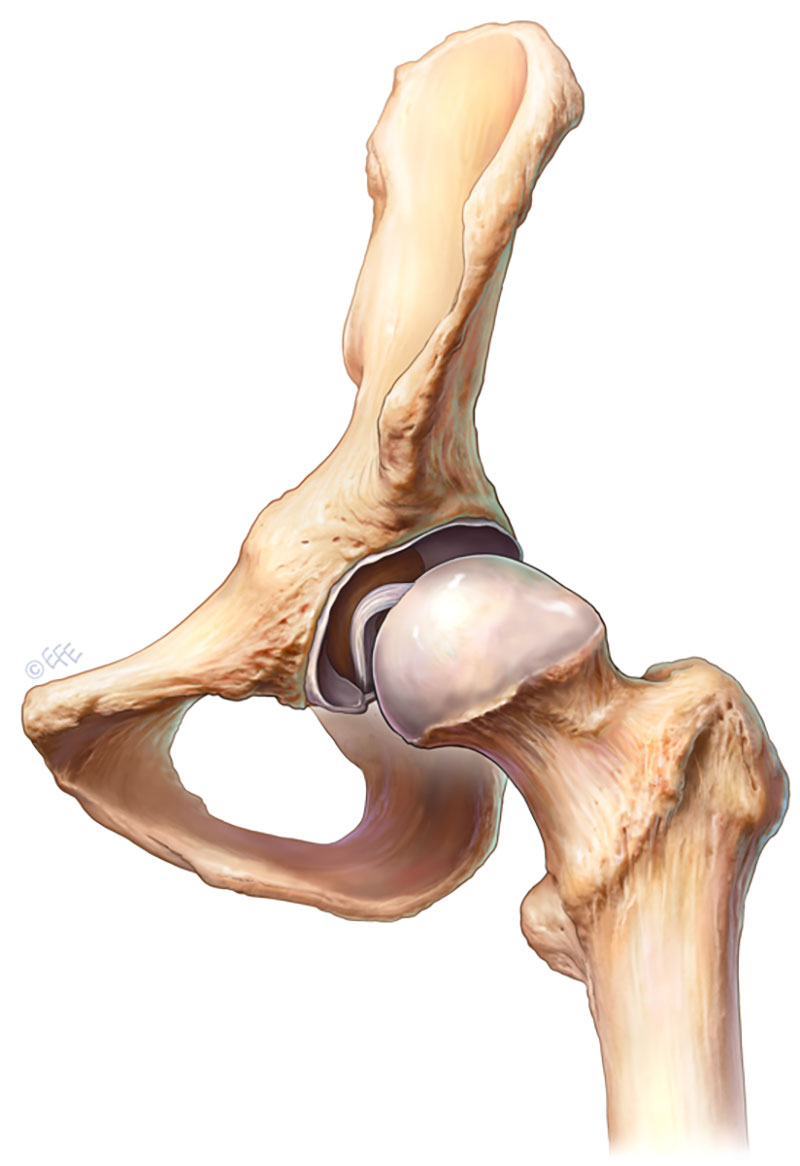
(Figure 1. Cam lesion on femoral head & neck (hipbone))
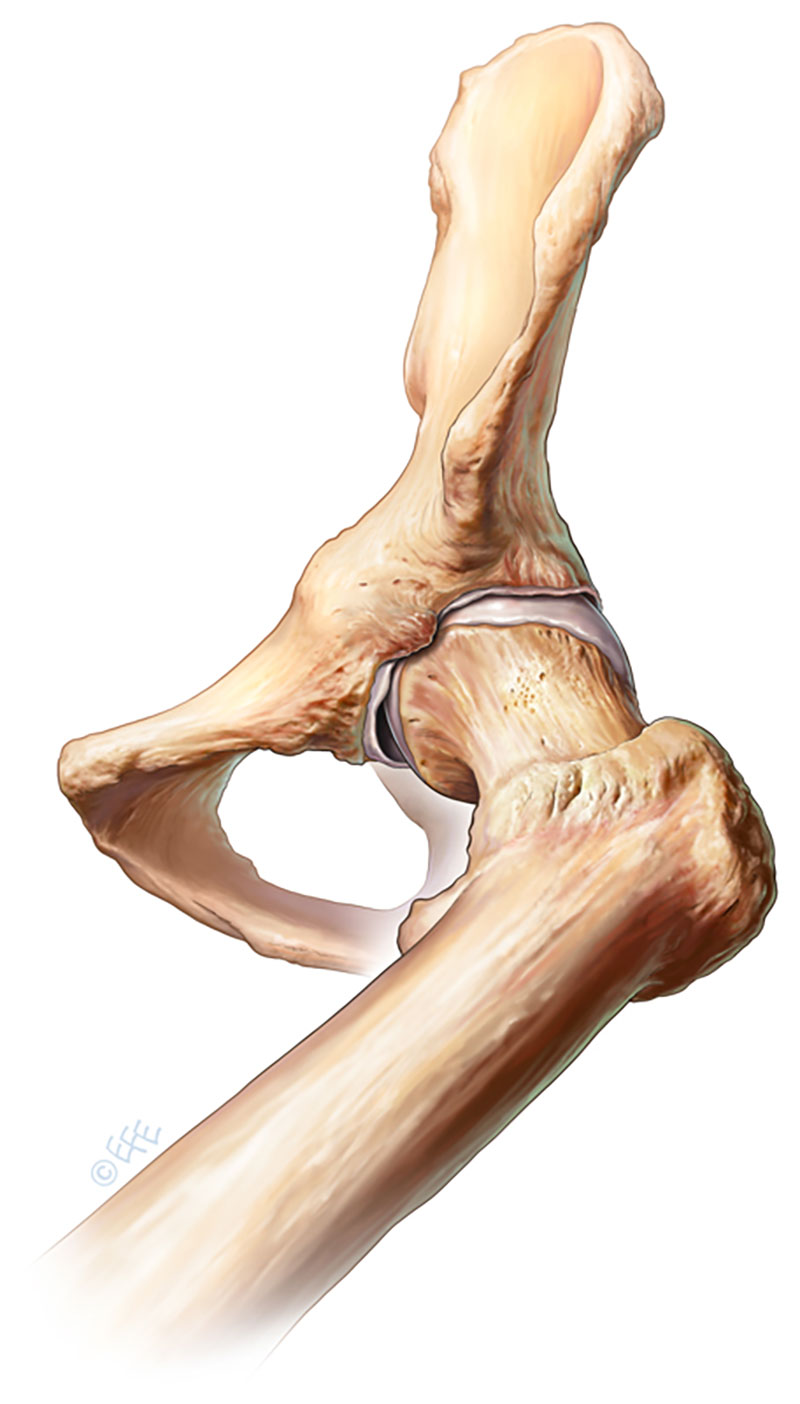
(Figure 2. Pincer lesion on acetabulum (socket))
Pathology outside of the joint may also be contributing to your pain e.g. Tendonitis of the surrounding muscles, inflammation in a bursa (fluid-filled sac), osteitis pubis or even a hernia. Clinical evaluation of your problem in combination with appropriate X-rays, CT and/or an MRI scan helps to establish the cause of your pain prior to surgery being undertaken.
SURGERY
Hip arthroscopy is performed in the operating theatre under a Spinal anaesthetic. Whilst asleep you are rolled onto your side and the legs are placed into a traction device to distract the affected joint and allow entry of the arthroscope.
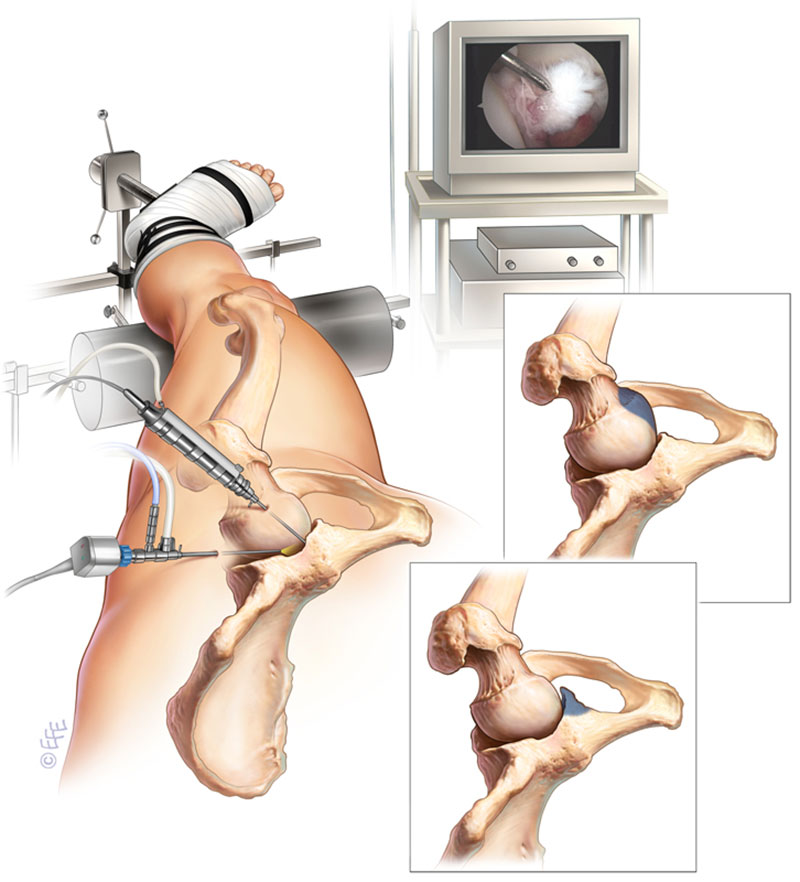
(Figure 3. Position during surgery (cam and pincer depicted on insets))
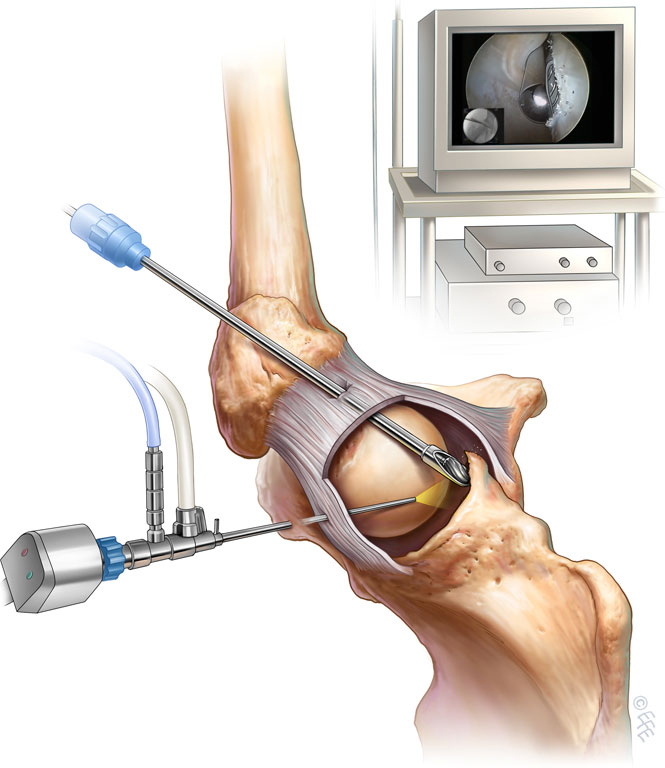
(Figure 4. A burr is used to remove a pincer lesion)
X-ray imaging is used in the operating theatre to confirm the site of your pathology and correct positioning of the arthroscope and working instruments. Usually, only 2 small incisions are made on the outer aspect of the hip to allow the instrument placement but occasionally a 3rd incision may be required to complete the procedure.
The common pathology of impingement (either cam or pincer) is treated via burring away of the bony bump (figure 4) plus repair of the torn cartilage (labrum).
The procedure usually takes approximately 1 hour to complete, whereupon the joint is infiltrated with a local anaesthetic prior to you exiting the operating room. Following an overnight stay in hospital, you will be discharged home fully weight bearing on the affected hip, using crutches for support.
POST SURGERY
Post-operative physiotherapy follow-up will be arranged and most patients can expect to be walking comfortably within 4-7 days. You should refrain from driving for this same period. Physiotherapy is initially targeted at retraining and strengthening the small muscles around the hip responsible for its stability prior to retraining and strengthening the larger muscle groups of the hamstrings, gluteals and quadriceps. Return to work is dependent upon your occupation but generally is at the 1-week mark following surgery for sedentary occupations and 3 weeks for heavy manual labouring work. Running and jumping activities should not be undertaken for 10-12 weeks with most patients ready to return to sporting activity soon thereafter.
RISKS
The complications of hip arthroscopy should be discussed with your surgeon prior to the procedure but may include those related to the anaesthetic e.g. nausea and vomiting, allergic reaction to the drugs, throat pain or swelling, and damage to the teeth. Complications related to the arthroscopy may include infection, deep venous thrombosis (DVT) and pulmonary embolism (PE), numbness in the anal, genitalia or inner thigh regions, and/or bruising and swelling in the same areas.
CONCLUSION
Hip arthroscopy is a safe procedure and provides good symptomatic outcomes for the pathologies listed above.
Please discuss the specifics of your particular condition with your surgeon.
Note: These notes have been prepared by orthopaedic surgeons. They are general overviews and information aimed for use by their specific patients and reflect their views, opinions and recommendations. This does not constitute medical advice. The contents are provided for information and education purposes only and not for the purpose of rendering medical advice. Please seek the advice of your specific surgeon or other health care providers with any questions regarding medical conditions and treatment.
The operation of a total hip replacement is a well established, long lasting procedure for relieving the pain involved with hip arthritis. This type of surgery has been used effectively now for over 40 years and remains the treatment of choice to achieve an excellent quality of life for sufferers of hip arthritis.
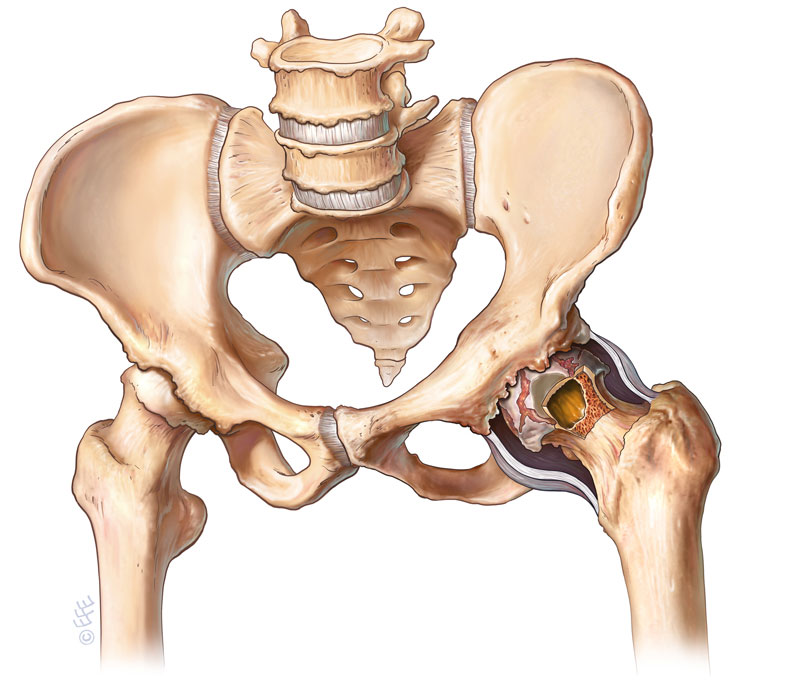
(Left Hip Arthritis)
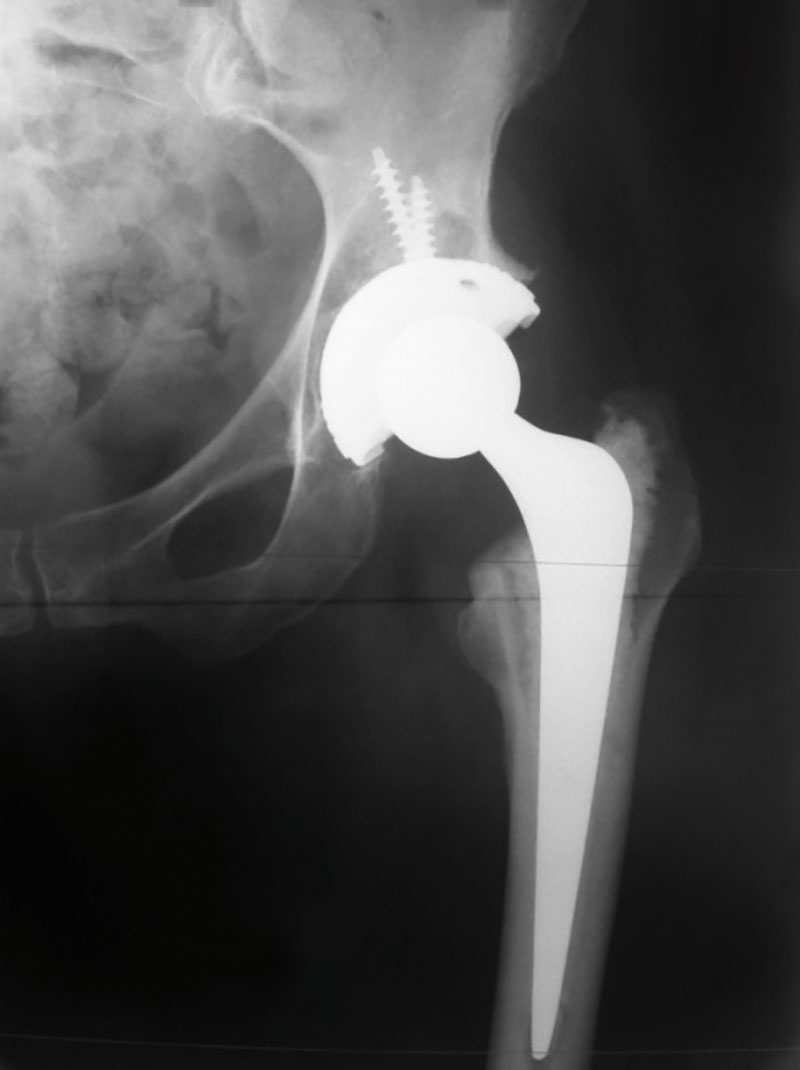
(Left total hip Replacement post-operative X-ray)
THE PROCEDURE
ANAESTHETIC
The type of anaesthetic that is used for the procedure will vary according to each patient’s co-existent medical conditions and also your wishes. Our group of anaesthetists are all competent in both general and regional (spinal) anaesthetics and will discuss with you prior to the procedure the benefits and risks of each technique.
SURGERY
Through an incision approximately 12-15cm long centred over the side of the hip and curving gently towards the buttock, the hip joint can be entered with minimal trauma to the surrounding muscles. The hip is dislocated and the femur bone is cut through its neck to expose both the pelvic and leg sides of the joint. Depending upon the quality of the bone and the age of the patient either a cemented or cementless component is fixed to the pelvis and similarly to the femur. The ball and socket mechanism of the joint is then reconstructed with either a metal on plastic (polyethylene) articulation or ceramic on ceramic articulation. Computer navigation may be used to ensure that the leg length obtained is correct and the orientation of the components is optimal to provide for maximum range of motion of the new hip.
Following the surgery you will be able to mobilize fully weight bearing on the hip the day after the procedure. You will be aided by the physiotherapist and nursing staff and taught how to safely use a frame initially and then graduate onto crutches.
Your hospital stay will be between 5-7 days and depending upon your home supports and progress.
Most people will be able to dispense with their crutches approximately 4-6 weeks following the surgery. During this time period you should sleep flat on your back, not cross your legs and use a seat raise for the toilet. These precautions will be emphasised by the physiotherapist during your hospital stay.All our patients are routinely put on home based physiotherapy post discharge.
AFTER DISCHARGE
Driving the car is not allowed for 6 weeks following the surgery and car travel as a passenger should be minimised during this period. These restrictions minimise the chance of the hip dislocating whilst the muscles and soft tissues around your hip heal.
At 6 weeks following the procedure you will be reviewed by your surgeon. Most patients are then given the all clear to return to recreational walking, swimming, cycling, golf, tennis, bowls, gymnasium workouts and other recreational pursuits as desired. It is not advised that you undertake running or jumping activities following a hip replacement.
FREQUENTLY ASKED QUESTIONS
What are the risks involved with the procedure?
There are general risks associated with any surgery, these are those of the anaesthetic (please speak to your anaesthetist prior to the operation), bleeding, blood clots (deep vein thrombosis (DVT) and pulmonary embolization (PE)), infection and vascular injury. Specific to the surgery are the risks of dislocation of the hip prosthesis, leg length inequality, fracture of the pelvis or femur, wear and loosening of the implants, audible ‘squeaking’ of the articulating components (ceramics), nerve injury.
When can I return to work?
Most people should be able to return to work at 6 weeks post-surgery. This may be extended if you perform a job involving heavy manual labour.
When can I resume sexual activity?
Sexual intercourse can safely be undertaken 6 weeks following the surgery.
How long do I need to keep taking pain-killing medicine for?
When you leave the hospital you will be given tablet analgesia for pain. You should take this for as long as you have pain when walking or at night. Most people are able to cease analgesics by 4 weeks following the surgery.
Do I need to do physiotherapy when I go home?
You will be given a sheet of exercises from the physiotherapist when you leave the hospital. You should do these exercises as instructed. You do not need to visit a physiotherapist once discharged.
Note: These notes have been prepared by orthopaedic surgeons. They are general overviews and information aimed for use by their specific patients and reflect their views, opinions and recommendations. This does not constitute medical advice. The contents are provided for information and education purposes only and not for the purpose of rendering medical advice. Please seek the advice of your specific surgeon or other health care providers with any questions regarding medical conditions and treatment.